Greater Trochanteric Pain Syndrome (GTPS) causes hip pain due to damage in the gluteal tendons. Focused Extracorporeal Shockwave Therapy (F-ESWT) has shown success in reducing pain and aiding tendon recovery. However, traditional monitoring methods rely heavily on subjective feedback.
This article explores how Shear-Wave Elastography (SWE) and Inertial Motion Sensing (IMU) provide objective data to track recovery. SWE measures tendon stiffness, offering precise insights into healing, while IMUs monitor hip mobility and movement patterns. Together, these tools allow clinicians to evaluate both structural and functional recovery, ensuring better treatment outcomes.
Key Takeaways:
- SWE: Quantifies tendon stiffness, detecting healing progress early.
- IMU: Tracks hip mobility, identifying movement issues during recovery.
- Combined use offers a detailed view of tendon health and functionality.
This integrated approach bridges the gap between imaging and functional recovery, helping clinicians make informed treatment adjustments for GTPS patients.
How Shear-Wave Elastography Measures Tendon Elasticity
What is Shear-Wave Elastography?
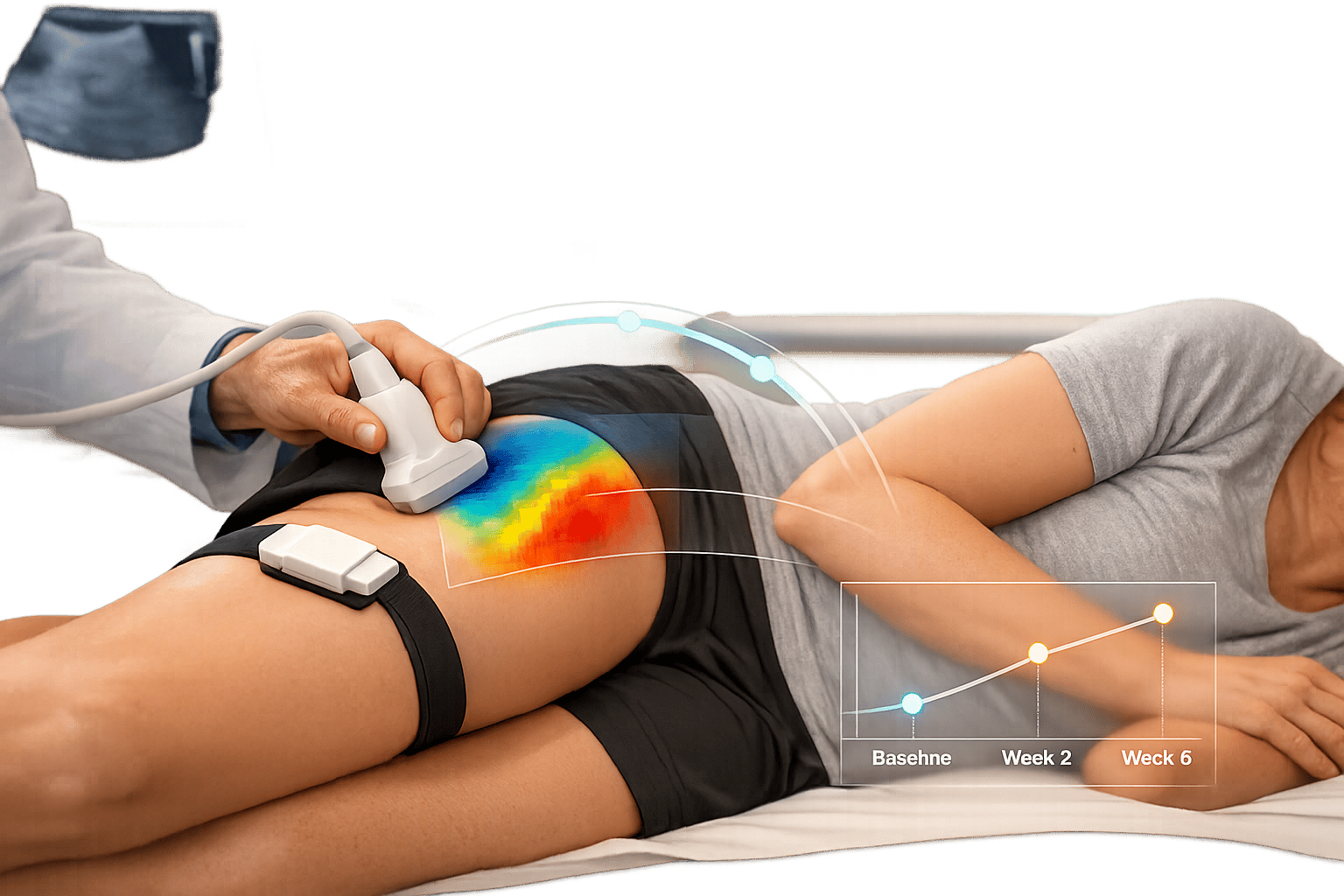
Shear-wave elastography (SWE) is a non-invasive imaging technique that evaluates the stiffness or elasticity of soft tissues, including tendons, by measuring the speed at which sound waves travel through them. Unlike traditional ultrasound, which focuses on structural imaging, SWE provides quantitative data – measured in kilopascals (kPa) or meters per second (m/s) – offering clinicians precise and objective metrics rather than relying on subjective visual interpretation.
The process involves generating shear waves using focused acoustic pulses, which are then tracked with ultra-fast imaging. Within just 30 milliseconds, these speeds are translated into a color-coded map that represents tissue stiffness [3]. Stiffer tissues allow shear waves to travel faster. Because tendons have a highly organized structure, measurements taken along their long axis typically show higher stiffness values compared to readings across the fibers. Healthy tendons generally exhibit a uniform stiffness pattern (blue or green on most color scales), while damaged tendons display softer areas (red or yellow), often caused by disrupted collagen fibers and fluid buildup [3][4].
"SWE is considered to be more objective, quantitative, and reproducible than compression sonoelastography with increasing applications to the musculoskeletal system." – Mihra S. Taljanovic, MD, PhD, FACR, University of Arizona [5]
This ability to produce precise, measurable data makes SWE an essential tool for monitoring tendon health, particularly during treatments like shockwave therapy.
Using SWE to Assess Tendon Health
SWE’s capabilities extend beyond imaging, providing critical insights into how tendons remodel during recovery. A notable study conducted by Yingqi You and Jia Hou at Sichuan Province Orthopedic Hospital in March 2026 utilized SWE to evaluate 60 patients with acute muscle and tendon injuries. Their findings revealed that injured tendons initially showed markedly lower stiffness values compared to healthy tissue (P < 0.001). However, these values improved steadily, nearly reaching healthy levels by week 12 [6].
One of SWE’s standout features is its predictive accuracy. Measurements taken as early as 4 weeks into recovery showed a strong correlation (r = 0.78, P < 0.001) with full functional recovery by week 12 [6]. This allows clinicians to gauge the effectiveness of treatment early, without waiting months for visible results. Combining SWE with high-frequency ultrasound has shown impressive diagnostic performance, achieving an Area Under the Curve (AUC) of 0.94, with a sensitivity of 91.7% and specificity of 88.3% [6].
"SWE-derived speed of sound measurements offer objective biomechanical markers for monitoring treatment response and assessing recovery outcomes, which may help inform return-to-activity decisions." – Jia Hou, Department of Functional Examination, Sichuan Province Orthopedic Hospital [6]
SWE can detect subtle changes in tendon mechanics before they become apparent on traditional ultrasound [4][6]. As shockwave therapy promotes collagen synthesis and cellular growth, the resulting improvements in tendon structure – such as increased density and organization – lead to higher shear wave speeds. This provides a reliable, quantifiable measure of healing, offering a more robust assessment than simply relying on patient-reported symptoms.
sbb-itb-ed556b0
Inertial Motion Sensing for Hip Mobility Tracking
How Inertial Motion Sensing Works
Inertial motion sensing works hand-in-hand with shear-wave elastography to deliver valuable insights into hip mobility during recovery. At the core of this technology are Inertial Measurement Units (IMUs) – small, wearable sensors that gather detailed movement data. These sensors use a trio of tools: accelerometers to measure gravity, gyroscopes to capture angular velocity, and magnetometers to determine horizontal heading [8]. Together, these components create a comprehensive picture of orientation, allowing clinicians to monitor hip mobility with an accuracy of 3 to 8 degrees, comparable to high-end stereophotogrammetry systems [8]. This level of precision is especially useful in assessing pelvic mechanics during rehabilitation.
For patients with Greater Trochanteric Pain Syndrome (GTPS), IMUs are particularly effective in tracking frontal plane pelvic mechanics, which are often affected by hip abductor weakness or discomfort. They can identify biomechanical issues like the Trendelenburg sign or compensatory trunk lean [7]. By analyzing pelvic tilt and lateral translation during movements such as transitioning from double-leg to single-leg stance, IMUs can uncover abnormalities that might go unnoticed in traditional evaluations.
"Movement system assessments are evaluations of biomechanics during functional activities providing insight into faulty movement patterns allowing clinicians to tailor treatment interventions to address identified impairments." – Ashley E. Disantis and RobRoy L. Martin [7]
IMU Benefits for GTPS Recovery Monitoring
IMUs bring more to the table than just precise movement detection – they offer significant advantages for tracking recovery in GTPS patients. Unlike patient-reported outcomes, which can be subjective, IMUs deliver objective, measurable data on joint angles and movement patterns. This is particularly useful for GTPS recovery, where the majority of patients (86%) are women, with an average age of around 61 years [1]. Because these sensors are lightweight and non-intrusive, they allow for continuous tracking during everyday activities or at-home exercises, eliminating the need for frequent laboratory visits [8].
Clinicians rely on IMU data to monitor critical movements like single-leg stance and stair climbing. Stair ascent, for example, is a key activity for analysis. Patients with gluteal tendinopathy are shown to be 4.5 times more likely to experience a significant hip adduction moment and increased pelvic translation at heel strike compared to healthy individuals [7]. By tracking these metrics, IMUs enable clinicians to remotely oversee recovery progress after treatments like shockwave therapy. This allows for real-time feedback and tailored adjustments to rehabilitation plans [8]. Combined with traditional pain assessments, IMU data offers a comprehensive view of recovery, focusing not just on reduced pain but also on restoring full function.
Shockwave Therapy for Tendon & Bone Injuries | Weill Cornell Medicine
Combining SWE and IMU for Complete GTPS Monitoring
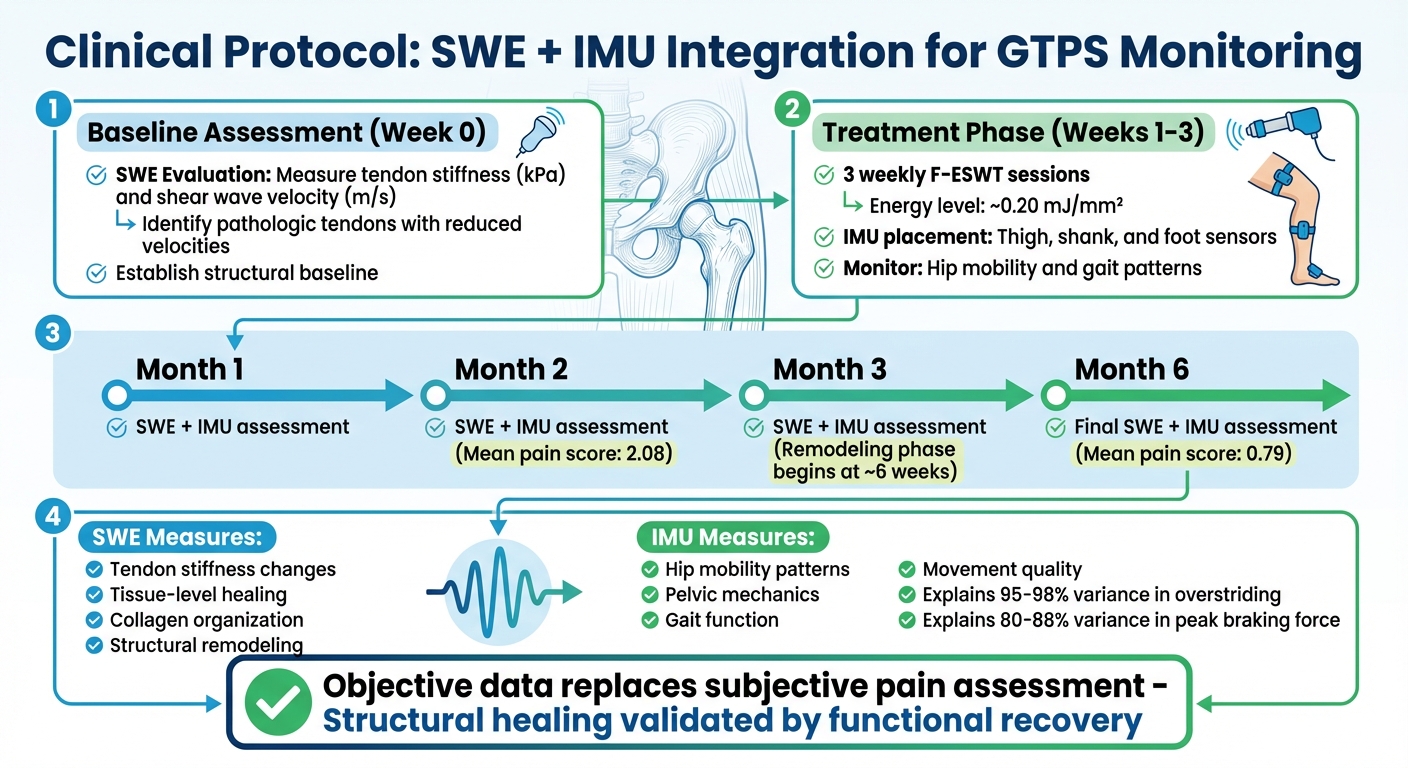
SWE and IMU Integration Protocol for GTPS Monitoring After Shockwave Therapy
Clinical Protocols for Using SWE and IMU Together
Using SWE (Shear Wave Elastography) and IMU (Inertial Measurement Units) together creates a comprehensive system for monitoring both the structure and function of tendons. The process starts with a baseline SWE evaluation to measure tendon stiffness (in kilopascals) and shear wave velocity (in meters per second). Pathologic tendons, which often exhibit reduced velocities, can be identified through this initial assessment. This structural data provides a clear starting point before initiating shockwave therapy.
After the baseline evaluation, patients undergo three weekly sessions of focused shockwave therapy, delivered at approximately 0.20 mJ/mm² [2]. During the recovery phase, IMUs are placed on the thigh, shank, and foot to monitor hip mobility and overall gait patterns [11]. Follow-up assessments are conducted at 1, 2, 3, and 6 months, utilizing SWE to observe tendon remodeling and IMUs to track functional movement [2][11]. This timeline aligns with the remodeling phase, which typically begins around six weeks after treatment [9]. This structured protocol bridges the gap between imaging results and functional improvements.
"SWE is a relatively recent modality that may increase sensitivity and diagnostic accuracy of conventional ultrasound imaging promoting early detection of tendinopathy." – D. Albano, Researcher [10]
Benefits of Using Both Technologies
By combining SWE and IMU, clinicians gain a more complete understanding of the healing process. This approach replaces subjective pain assessments with objective data on both tendon structure and function [2]. SWE highlights tissue-level changes, while IMUs reveal whether these changes lead to improved movement patterns. For instance, sagittal segment angles measured with IMUs can explain 95% to 98% of the variance in overstriding during running, as well as 80% to 88% of the variance in peak braking force [11]. These strong correlations help clinicians ensure that structural healing observed in imaging corresponds with meaningful functional recovery in daily activities.
Clinical Applications at Portland Chiropractic Group
How Portland Chiropractic Group Uses SWE and IMU
Portland Chiropractic Group combines shear-wave elastography (SWE) and inertial motion sensing (IMU) with focused shockwave therapy to treat greater trochanteric pain syndrome (GTPS). This approach connects detailed tendon imaging with functional recovery, reflecting a commitment to data-driven care. The process starts with a thorough evaluation to identify patients dealing with persistent hip pain, gluteal tendinopathy, or similar musculoskeletal challenges. Before starting treatment, the clinic carefully screens for potential contraindications such as blood clotting disorders, infections, nerve conditions, or recent steroid injections [12].
Once patients are cleared, the clinic customizes its focused extracorporeal shockwave therapy (F-ESWT) protocol based on how each individual responds. Adjustments are made in real-time following each session to ensure optimal outcomes [12]. To measure progress, the team uses tools like the Numeric Rating Scale (p-NRS) and the Lower Extremity Functional Scale (LEFS), which provide accurate insights into improvements in hip mobility and limb function [1]. Formal assessments are conducted at two- and six-month intervals to monitor the shift from immediate pain relief to long-term tendon remodeling [1]. This structured approach ensures that outcomes are both measurable and tailored to each patient.
Patient Benefits of Advanced Monitoring
With these advanced techniques, patients benefit not just from pain relief but also from clear, objective tracking of their progress. Those undergoing this integrated care approach often experience notable reductions in pain over the short and medium term. Research shows that F-ESWT can lower mean pain scores from 2.08 at two months to 0.79 at six months, while also encouraging cell growth and collagen production in human tenocytes [1]. This supports true tendon healing rather than just masking symptoms.
The use of SWE and IMU technologies provides tangible progress markers, which help keep patients engaged and confident in their recovery. While pain and mobility improvements are often noticeable within one to three sessions, the full biological effects can take up to three months to unfold [12]. This timeline helps set realistic expectations, showing patients that recovery is a gradual process, with structural tendon changes aligning with improvements in daily function.
Conclusion
Combining shear-wave elastography (SWE) with inertial motion sensing (IMU) provides a well-rounded way to monitor recovery in patients with greater trochanteric pain syndrome. SWE quantifies tendon healing by measuring stiffness and elasticity, while IMU captures how these structural changes improve hip mobility and gait function. Together, these tools deliver objective data to guide treatment decisions.
Studies have shown notable recovery outcomes when focused extracorporeal shockwave therapy (F-ESWT) is paired with targeted exercise programs [2]. Building on this evidence, Portland Chiropractic Group emphasizes research-driven care. By using SWE to track tendon remodeling and IMU to assess functional recovery, they can fine-tune therapy plans, especially for chronic cases where conventional methods might fall short. This dual-monitoring approach ensures treatment progress is validated and adjustments are made when needed.
For patients with ongoing hip pain, this integrated strategy provides clear, measurable progress markers. Seeing tangible improvements in both tendon health and mobility helps patients set realistic goals and stay motivated throughout their recovery journey.
FAQs
Is SWE safe, and does it hurt?
Shear-wave elastography (SWE) is a non-invasive and painless diagnostic method when safety protocols are properly followed. This technique prioritizes patient comfort, making it an accessible option for various medical evaluations.
Where are the IMU sensors placed, and can I wear them at home?
The IMU sensors are placed directly on the tendon or nearby areas. These sensors are specifically designed for home use, making it easy to track your progress conveniently.
How soon can SWE and IMU data show improvement after shockwave therapy?
Studies show that shear-wave elastography (SWE) and inertial motion sensing (IMU) data often improve within just 1 to 2 months following shockwave therapy. By the 2-month point, patients commonly experience noticeable pain relief and tendon remodeling.
Related Blog Posts
- Shockwave Therapy: What to Expect During Treatment
- Tendinopathy: The Interplay between Mechanical Stress, Inflammation, and Vascularity
- Utility of clinical tests to diagnose MRI-confirmed gluteal tendinopathy in patients presenting with lateral hip pain
- Effectiveness of fascial manipulation® versus eccentric training with static stretching on patellar tendinopathy – A randomized clinical trial


Comments are closed